New Mother - 0 to 6 months baby
Article
Breastfeeding Guide: Before, During & After Birth
Nov 4, 2016
5 mins
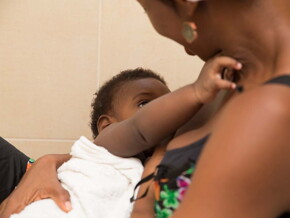
As you are aware, breast milk provides the perfect food for your baby through her first six months and even after you introduce other foods. Knowing what to expect before you give birth can help you formulate a mental ‘game plan’ so you can enjoy every moment that you’re nourishing and nurturing your baby.
Here are some tips for a successful start:
Before the birth
- Gather support. Recruit as many breastfeeding supporters as you can, such as your partner, friend, mother, sister or anyone who will cheer you on to breastfeed as you learn more about it.
- Talk to your doctor about breastfeeding. Let your doctor or nurse know about your intention to breastfeed and find out what lactation support services are offered by their practice, now and after your baby is born.
- Get prenatal breast care. Have a discussion with your doctor about expected breast changes, previous breast surgeries, hormone concerns (including thyroid issues or diabetes) and any other health questions that you think may relate to breastfeeding. This discussion may help you to prepare for and manage special breastfeeding situations.
- Ask about your hospital’s breastfeeding procedures for newborns. See if there is a certified lactation consultant that can visit with you before you leave the hospital.
- Purchase a breast pump. Breast pumps are meant as an alternate way of expressing your breastmilk when your baby is unable to nurse directly such as when you may go back to work or school.Decide what type of pump to purchase based on how much you will need to pump, from less expensive manual pumps for occasional use to more expensive, more efficient electric pumps, through to hospital grade pumps for frequent, extended use.Understand how to clean your pump thoroughly as you will need to clean it prior to first use and after each use to reduce bacteria risks for your baby.
- Get connected with community support. Reach out and attend a prenatal breastfeeding class or breastfeeding support group. This will give you an idea of what to expect and connect you with some possible future resources.
- Pack a checklist in your hospital bag. Along with your pyjamas and slippers, include a checklist of your breastfeeding-related requests to discuss with the hospital staff. An example checklist is included below.
When you’re admitted to the hospital
- Tell staff you plan to breastfeed. Ask the labour and delivery nurse to notify the nursery that you will be breastfeeding.
- Note breastfeeding on chart. Request that your baby rooms in with you continuously and have a note be made on the chart that your baby should not receive any bottle feedings, unless medically needed. If separated from your baby, she should be brought to you when showing the first signs of hunger.
- Request breast-only feedings. Request supplements not be given to your baby unless medically necessary.
- Request to see a lactation consultant. A lactation consultant will be able to help you with positioning, latch-on and other questions that you may have before leaving the hospital.
After your baby is born
- Breastfeed as soon as possible. The World Health Organisation (WHO) recommends that mums breastfeed as soon as possible after birth, preferably within the first hour. Your baby can benefit right away from the easy-to-digest proteins, vitamins, and minerals, and protective antibodies in colostrum, the yellowish, translucent fluid your breasts secrete until your mature milk transitions over the next two to three days.
- Practice skin-to-skin. Let your labour and delivery team know your wish to lay your baby on your chest, skin-to-skin, right after birth and until the first feeding is complete. Do this as often as you’re able to during the first few months to help your baby have calm feedings, and help you have a good milk supply.
- Feed when hungry. Breastfeed your baby whenever she’s hungry, which should be at least 8 to 12 feedings in a 24-hour period.
- Use both breasts. Breastfeed from both breasts to equalize the breast milk production in your breasts. Allow your baby to end the feeding on the first breast before offering the second. If he refuses the second breast, offer that breast first at the next sign of hunger.
- Don’t worry about time limits. It’s best not to set a specific feeding time limit but rather make sure your baby is feeding effectively until satisfied. Some babies eat quickly; others take their time.
- Look for hunger signs. It’s best that you don’t wait until your baby begins to cry to breastfeed. Instead, look for signs of hunger such as increased alertness, the rooting reflex (searching for a nipple) or the sucking reflex.
- After a C-section. Even if you’ve had a caesarean section, it’s still important to breastfeed as soon as possible. You may find the “rugby hold” will be the best way because it puts less pressure on your incision. (Imagine the way a rugby player carries a ball, and you’ll get the idea.)
Before you leave the hospital
- Ask a pro. Ask to have a lactation consultant observe you feeding your baby and make suggestions.
- Learn how to hand-express. Hand-expressing your milk may be all that is needed to soften your breast if you become overly full when your milk transitions to mature milk in two to three days. This will help your baby latch on easier.
- Get names and numbers. Get the names and phone numbers of the hospital’s breastfeeding consultants so you can call for advice or answers once you and your baby are home.
At home
- Call with questions. If you have questions or concerns about breastfeeding, ask your doctor, lactation consultant, breastfeeding peer counsellor, or a friend or family member who has successfully breastfed for guidance.
- Do not wait to get support if you feel pain or discomfort while trying to breastfeed.
Hospital Breastfeeding Checklist
- Tell staff you plan to breastfeed.
- Ask to have ‘breastfeeding’ be put on your and your baby’s chart.
- Request to room-in with your baby. If not possible, ask that baby be brought to you at the first sign of hunger
- Remind staff that you’d like to do skin-to-skin immediately after birth.
- Ask that your baby not be given a pacifier or formula unless medically necessary.
- Request to see a lactation consultant to observe a feeding.